How Diabetes and High Blood Pressure Are Linked
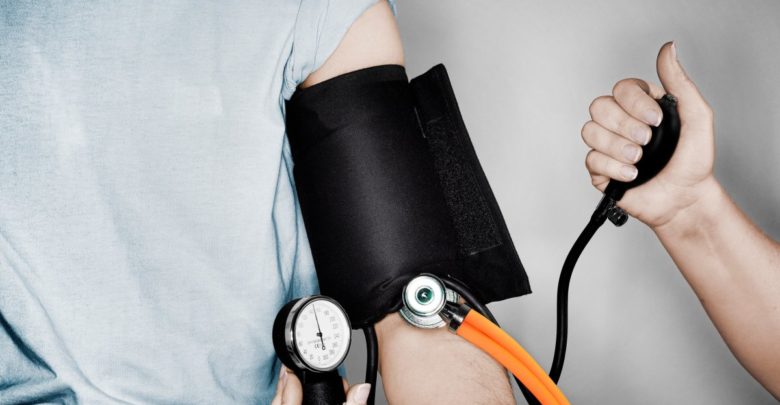
High blood pressure—also known as hypertension—and Type 2 diabetes are two of the most common medical conditions in the U.S. They often co-occur. Some research has found that 85% of middle-aged or older adults who have Type 2 diabetes also have hypertension, and both conditions elevate a person’s risk for heart disease, stroke, and kidney disease.
The increased risks can be serious and even fatal. Researchers have found that people with Type 2 diabetes are up to four times more likely to develop cardiovascular disease than those who don’t have the condition. Heart disease is twice as common in people with diabetes. People with diabetes and high blood pressure are more likely to experience strokes, kidney disease, or other fatal complications.
These conditions often appear in conjunction. Although experts are not able to pinpoint the exact cause, they believe excess weight could play an important role. Many people who have hypertension and Type 2 diabetes also have obesity, and this “triumvirate,” as some researchers have termed it, is associated with metabolic and endocrine problems that overlap and promote disease. “Obesity seems to be fertile soil for both,” says Dr. Srinivasan Beddhu, a professor of internal medicine at the University of Utah School of Medicine.
Also, the sheer commonness of hypertension all but ensures that most people with Type 2 diabetes will end up with both diseases. Hypertension affects approximately half of Americans, with the percentage increasing as we age. “It can develop as early as [ages] 30 to 42, but in most cases, by the time you’re in your 50s, it’s there,” says Dr. George Bakris, a professor of medicine at the University of Chicago. Bakris states that Type 2 diabetes often occurs before hypertension, but it is becoming more common among young people and children. It’s more important than ever to keep an eye out for both conditions, perhaps especially if you’re overweight or obese.
Experts explain the combination of high blood pressure (and Type 2 diabetes) and how they can be managed and reduced.
Continue reading: These new developments could make it easier to live with type 2 diabetes
The connection
The circulatory system sends blood into the body every time the heart beats. Between beats, blood is pumped into the heart. A person’s blood pressure refers to two different but related measurements of this cycle. The first measurement, called systolic, refers to the pressure within the arteries as blood is pumped out by the heart. The diastolic (or blood pressure) measurement is when blood is flowing freely through the arteries. They are often presented in combination and almost always fluctuate together. In the U.S., blood-pressure scores higher than 130/80 mm Hg are considered hypertensive.
Bakris says hypertension is often called a “silent killer” because it may cause no symptoms. Even when a person’s blood pressure is dangerously high, the symptoms that develop are so common and nonspecific—meaning they turn up for all sorts of reasons—that you may not connect them with high blood pressure. These symptoms include blurry vision, dizziness, headaches and blurry eyes. By the time they set in, a person’s blood pressure may have been elevated—and doing damage—for several years. Which kind of damage can they cause? What can cause blood pressure to rise? Stress on your kidneys, and other organs can also be increased by high blood pressure.
Type 2 diabetes is a medical condition defined by high blood-sugar levels. These high levels are caused by problems related to insulin, which is a hormone that signals to the body’s cells that they need to absorb blood sugar. In people with Type 2 diabetes, the cells become “resistant” to insulin, meaning they do not properly absorb blood sugar. As with hypertension, the early symptoms of Type 2 diabetes—frequent urination, blurry vision, dramatic hunger spikes—may not raise immediate red flags. If someone isn’t staying on top of their doctor’s appointments, they may not be aware that one or both of these conditions is present.
What happens when these conditions are combined in ways that can lead to serious health issues? “Both affect the small blood vessels,” says Dr. Mattias Brunstrom, a hypertension specialist and physician researcher at Umea University in Sweden. “Diabetes affects the vessels in ways that make them stiffer, and high blood pressure impairs their function.” This stacking of arterial damage helps explain why the combination of the two conditions is associated with cardiovascular problems, including higher rates of heart disease and stroke.
At the same time, both hypertension and Type 2 diabetes may also promote higher-than-normal levels of blood sugar. High blood sugar levels can cause damage to the kidney cells, blood vessels and heart. Kidney disease—and ultimately kidney failure—is a common complication among people with both of these conditions. “If you have [systolic] blood pressure consistently above 180, within 12 to 15 years, you will be on dialysis,” Bakris says, referring to a medical procedure that removes, filters, and returns the blood to someone whose kidneys are no longer up to it. Elevated blood sugar caused by Type 2 diabetes further damages kidney cells, and increases the odds that the kidneys will struggle or fail to perform their job.
Although cardiovascular and renal problems are two of the most common complications, hypertension and Type 2 diabetes can cause or contribute to a wide range of health problems—from dementia to blindness. “Both affect the vasculature, which can impair the health of any organ system,” Brunstrom says.
These conditions can be managed effectively, reducing the risk to your health.
Continue reading: What the Truth is About Type 2 and Fasting
Here’s what you can do
Experts say that lifestyle modifications and prescribed drugs can often be combined to treat Type 2 Diabetes and hypertension.
“First, I would say that lifestyle changes are the basics of all disease management,” Brunstrom says. He re-emphasizes the strong associations linking hypertension and Type 2 diabetes to obesity, and the role excess weight plays in exacerbating many health complications. “Obesity or overweight is a huge driver of both these conditions, so weight management would be very crucial,” he says. “Diet, exercise—any way you can get your weight down is good.”
Even if you’re not losing weight, exercise is still beneficial. “It increases circulation around the body and improves function of the small vessels, which might get [blood] pressure down,” he says. “It might also improve the sensitivity to insulin and reduce glucose.” That’s all good stuff. Even short of sweaty exercise sessions, spending less time sitting or in a sedentary position—walking, for example, or doing chores around the house on your feet—may be helpful.
Brunstrom refers to the DASH eating plan, which has been approved by the National Heart, Lung, and Blood Institute (NHLBI) for managing hypertension. (DASH stands for “dietary approaches to stop hypertension.”) The DASH diet involves limiting your intake of saturated fats, which are common in red meat and fatty dairy products, and also cutting down on your intake of salt and sugary foods and drinks. The DASH diet encourages you to eat lots of vegetables and fruits. These eating habits are supported by other experts. “I always tell my patients to eat healthy, which means more fruits and vegetables, less red meat, fewer high-carbohydrate foods,” says the University of Utah’s Beddhu.
Recent research has shown the effectiveness of intermittent fasting in the treatment of Type 2 diabetes. These approaches involve limiting or eliminating all caloric intake for an extended period of time—usually 16 hours or longer. There’s evidence that they may be beneficial. People with mild to early diseases may also find them safe. “But if you have diabetes and are on medications, these diets can wreak havoc,” Bakris says. “If you want to try that, you need the help of a physician or accredited diabetes dietitian.”
The weight loss surgery option may be worth looking into. Research has shown that both adults and young people can get better control over their hypertension and diabetes with bariatric surgery. Some cases, particularly those that involve teenagers, have seen weight loss surgery eliminate the need to take medication or completely eradicate the disease.
Experts agree that prescription medication is almost always required to treat these conditions. “You can reduce your pill burden if you’re really good on the lifestyle side—so eating right, reducing sodium intake, exercising regularly,” Bakris says. “But even on the low end, most people with diabetes and hypertension are going to require four to six medications.”
Many others agree with the statement that pills cannot be avoided. “I always compare [taking] them to doing your taxes or brushing your teeth,” says Dr. Tom Brouwer, a cardiology resident and researcher at Amsterdam University Medical Centres in the Netherlands. “It’s not fun, but you need to do it.”
In the U.S., medical guidelines recommend that doctors aim to get people with both hypertension and diabetes down to blood-pressure scores below 130/80 mm Hg. There’s some ongoing debate about whether targeting even lower numbers would be beneficial. Brouwer has conducted research in this area, and he says that in many cases he’s a proponent of aiming for a systolic BP of 120. “If a patient tolerates it, I tend to try to lower their blood pressure all the way to 120,” he says.
Both Type 2 and hypertension can be treated with a variety of drugs. But two of the most popular options are angiotensin-converting enzyme inhibitors and angiotensin II receptor blockers, both of which help relax the arteries and so assist blood flow. These drugs are effective in hypertension and also protect your kidneys. These drugs include diuretics, which increase urine production.
Continue reading: Diabetes is more common in people with diabetes. What can you do to reduce the risk
“With these three drugs, an overwhelming majority of patients get to the target blood pressure,” Brouwer says.
For those at risk for hypertension, diabetes, or both, experts say that all the lifestyle measures above—a good diet, exercise, and maintaining a healthy weight—are among the best ways to lower your risks. By following your doctors’ drug recommendations and trying to live a healthier life, you can protect yourself from serious complications. “I tell patients: you can help yourself,” Bakris says. “But you have to put in the effort.”
Read More From Time




