When Pregnant People Should Get COVID-19 Vaccine
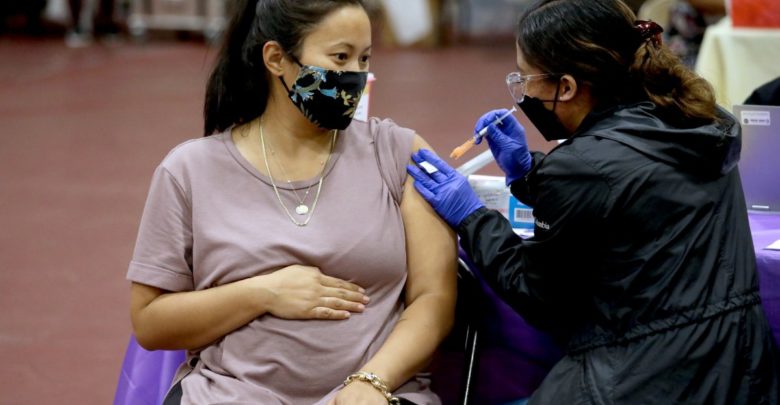
COVID-19 poses health risks during pregnancy for everyone involved. Pregnant people are at higher risk for severe disease, and the chances of negative outcomes for mother and baby—such as preeclampsia, preterm birth, and stillbirth—increase with infection. Pregnant women were not included in the initial vaccine trials. Many mothers-to-be were therefore hesitant about taking the vaccines when they first became available.
In the United States, thousands of pregnant women are now vaccinated. There is a wealth of evidence that vaccinating during pregnancy protects both mother and baby. The vaccine gives infants anti-SARS-CoV-2 antibodies, which reduces the likelihood of them being admitted to hospital with the disease. A June study also showed that 69% less people will be admitted to the hospital for the illness in the first six month of their lives.
The journal now publishes research Nature CommunicationsThe COVID-19 vaccine can be administered in three different trimesters. It has been shown on June 28 that there are measurable benefits for mother and baby.
Researchers from Massachusetts General Hospital and Brigham and Women’s Hospital analyzed the anti-SARS-CoV-2 antibodies of 158 women who were vaccinated during their pregnancies. Most received either Pfizer-BioNTech’s or Moderna’s vaccine, which both generated a superior immune response compared to Johnson & Johnson-Janssen’s shot. The strongest immunity to vaccines was seen in those who received an mRNA vaccination during the first and third trimesters. Antibody levels generated during second-trimester vaccination were somewhat weaker, which may be because pregnant people’s immune systems are more active during the first and third trimesters, and therefore may generate a greater response to the vaccine, says Dr. Andrea Edlow, a maternal fetal medicine specialist and physician scientist at Massachusetts General Hospital and Harvard Medical School, who co-authored the study.
The researchers also tested the levels of antibodies in women’s umbilical cords at birth, a measure that suggests how well mothers are able to transfer protection to their fetuses. The transfer of antibodies between mother and baby is most effective in the first and third trimesters. This suggests that infants whose mothers were vaccinated earlier in pregnancy receive COVID-19 vaccine antibodies immediately. However, the absolute number of antibodies transferred was highest if the mother was vaccinated during the second or third trimester, which may mean that babies whose mothers were vaccinated later in pregnancy were offered more protection—likely because mothers’ COVID-19 immunity waned over time. Edlow states that this data suggests the third trimester is the best time to receive a COVID-19 boost. The CDC also recommends that pregnant women get the Tdap vaccination for whooping cough to ensure their babies are protected after delivery.
Edlow says that while it’s important for unvaccinated women to get vaccinated as soon as possible, the study shows how to maximize the benefits for both mother and fetus. “If I were an unvaccinated pregnant person, I would definitely get vaccinated in the first trimester. But I would also probably use the opportunity then to be boosted in the third trimester,” says Edlow. (However, she emphasizes that during the pandemic, the priority is getting vaccinated as soon as possible, no matter what trimester you’re in.)
The study was kept small so that scientists could use in-depth methods to analyze the quality of the antibody production, but its size means that it can’t give a complete picture of how vaccines work in pregnant women, Edlow says. Scientists have now accumulated enough data to show that vaccines are safe and effective for pregnant women. Studies like these can be used by scientists to improve their knowledge of the mechanisms of immunity and COVID-19 antibodies during pregnancy. The long-term implications of this research will be to inform future COVID-19 vaccination recommendations during pregnancy.
“We can say with confidence to pregnant individuals at this point, it’s safe to be vaccinated in pregnancy, it doesn’t cause an increased risk of miscarriage, it doesn’t cause birth defects,” says Edlow. “It does protect the mother against severe disease and death, and it does protect against pregnancy complications.”
Because they weren’t included in this study, the results of this research don’t directly apply to pregnant persons who have already been fully vaccinated. Unless they have immunocompromised, the CDC does not recommend a second booster shot for pregnant women. Edlow stated that the guidance may change in time as COVID-19 periodic booster shots are expected to be more common.
Since the first shots were made, pregnant women are now more likely to get vaccinated. More data has been available showing that the vaccines have proven beneficial. Below are charts that show how the vaccine gap has narrowed between pregnant people and women who have not been vaccinated in the last year. But, it is less common for women trying to become pregnant to receive a booster than those who have not had one.
Edlow suggests that these women may have the opportunity to boost their chances of protecting their babies and themselves during pregnancy. It is not known if booster shots were given in the current study. Edlow recommends pregnant women get a booster vaccine when they become eligible. She suggests doing this after the 20-week mark.
However, Edlow adds that mothers should also weigh their individual risk of severe illness when deciding whether to get a booster sooner—since a mother’s health is a top priority during pregnancy. “The important message for pregnant people is: by protecting yourself, you’re doing the best thing that you can do to protect your baby,” she says.
Read More From Time





